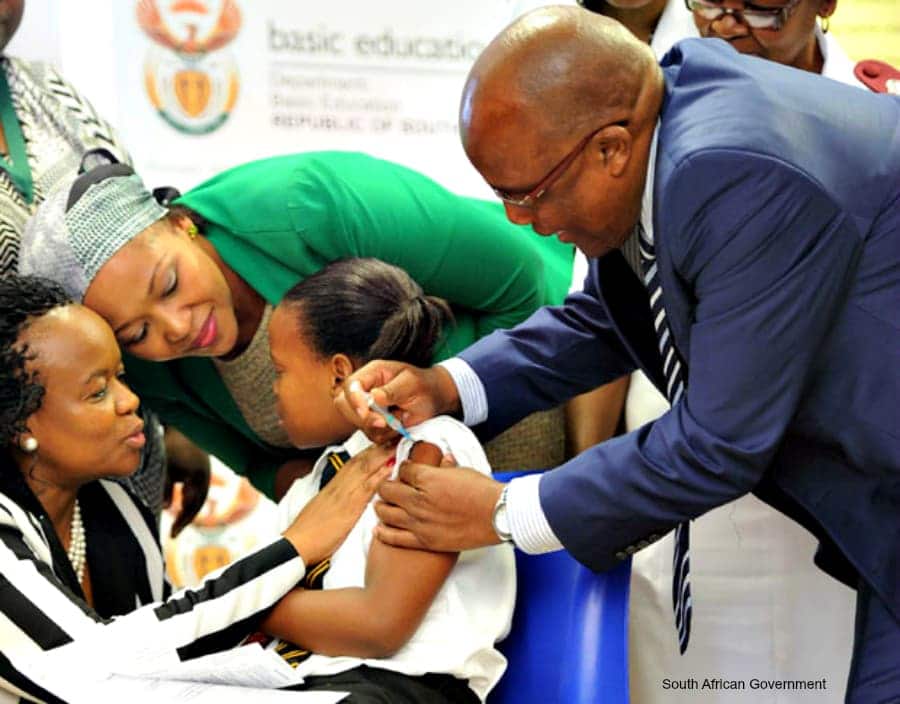
No turning back
For the past six weeks, health officials and specialist advisors have been
working late into the night to meet Tuesday’s (30 Sept) deadline set by
Cabinet to come up with a “detailed operational plan on an anti-retroviral
treatment programme”.
“It is as if we have finally woken up to the fact that we are in an
emergency. People are working as if we are a country at war,” says a source
close to the process.
While cynics say the urgency is being fed by the 2004 general election, few
in the HIV/AIDS field doubt that South Africa has reached the point of no
return on the provision of ARV drugs.
The Cabinet-driven programme has the potential to commute the death
sentences of approximately 1,2 million South Africans expected to develop
AIDS over the next seven years, and prevent 860 000 children from becoming
orphans.
It also has the potential to revitalise our health system and restore the
morale of health workers.
But if it is not implemented properly first time it will result in
drug-resistant HIV, which will effectively render useless the only weapon
the world has to fight the virus: anti-retroviral drugs.
A government-appointed task team headed by the Medical Research Council’s Dr
Tony Mbewu has been driving the process, assisted by experts from the
Clinton Foundation.
It has been a difficult time for the health department. Its director
general, Dr Ayanda Ntsaluba, left at the end of August while its HIV/AIDS
head, Dr Nono Simelela, has been hospitalised twice recently.
But, says Mbewu, “everything is on track” for Cabinet to get the final
report on the operational plan on Tuesday (30 September). Cabinet is likely
to take at least a week to respond to the report before it becomes public.
Treatment Action Campaign (TAC) secretary Mark Heywood says there is a
“seriousness within the task team, which is being thorough in its approach”.
TAC has made a submission to the team and is also helping some of the
provinces.
Aside from assisting provinces with their rollout plans, the task team has
been looking at staff capacity and training, laboratory services and drug
procurement. It has met a number of drug companies, including Cipla, the
Indian generic ARV manufacturer reputed to make the cheapest ARVs in the
world.
For once, there is significant financial backing for the rollout. Aside from
R4-billion set aside for HIV expenditure in the provinces, Treasury has made
available a conditional grant of R210-million for this financial year alone.
A lot more money is expected soon.
The beauty of conditional grants is that they are earmarked for specific
things and allow national government to inspect provincial operations to
make sure the money is being spent where it is supposed to.
Thus, the task team has been able to parachute a team into Mpumalanga to
assit with preparations for the rollout. This is something national
government has been unable to do in the past, despite the fact that the
province’s HIV/AIDS programme was virtually destroyed under former health
MEC Sibongile Manana.
While provinces have been able to select their own facilities, they have had
to ensure that these offer citizens “equitable access” to ARVs – in other
words, in both rural and urban areas.
As a result, most provinces have centred their rollout plans on district
hospitals. The general consensus is that doctors should be responsible for
prescribing the antiretroviral drugs. However, nurses will need to play a
significant role in both the assessment and ongoing management of the
patients on treatment.
Realistically, the ARV programme may well only start properly in the new
year when facilities have been prepared, staff have been trained and
patients are not likely to disappear over Christmas. However, Heywood says
sites that are ready should begin in November as “any delays will kill
people”.
For government’s Nono Simelela, the biggest challenges of the rollout are
“staff training, proper infrastructure and ensuring community understanding
of how to take ARVs”.
There are plans to set up provincial HIV/AIDS centres to train health
workers. Doctors with little practical experience of HIV/AIDS may also get
support via phone and email from HIV experts, to deal with drug side-effects
and the many complications that come with treating people with very weak
immune systems.
According to a Treasury-Health department report, by 2010 it will cost
between R16,9-billion and R21,4-billion, depending on drug prices, to treat
all AIDS patients.
Generic medicine can reduce costs massively. While government’s best
estimate of drug costs is R7 611 per patient a year for a combination of the
drugs 3TC, d4T and nevirapine, the newly formed Generic Antiretroviral
Procurement Project says it can treat people for R2 460 a year using generic
versions of the same drugs.
While foreign donor support is available at present, University of Cape Town
economist Professor Nicoli Nattrass says the necessary finances could also
be raised by increasing valued-added tax (VAT) by between three and seven
percent.
However, it is unlikely that 100% of those who need treatment will seek it.
In Botswana, for example, only 7 000 of the estimated 110 000 eligible
patients are on ARV treatment. While AIDS stigma is one barrier, some say
Botswana spent too little time raising public awareness about treatment
before offering the drugs.
If South Africa’s programme is to succeed, money will have to go into
improving infrastructure to ensure that drug supplies are stable and that
there is adequate laboratory support necessary for tests to monitor immunity
in the blood (CD4 counts) and viral loads. Extra staff will be needed and
current staff will need training. These measures will benefit all South
Africans using public health.
Health workers’ morale will be boosted as they will no longer be helpless
when faced with destitute AIDS patients.
“This is a once in a lifetime opportunity,” says Dr Douglas Wilson, medical
specialist at Greys Hospital in Pietermaritzburg. “What is happening in
South Africa has never happened anywhere else in the world. In the future,
health workers should look back on this rollout as the highlight of their
professional careers,”
Wilson, who has treated AIDS patients at Somerset Hospital in the Western
Cape over a number of years, says “you can get addicted to watching the
progress of your patients on ARVs, as they put on weight and go back to
leading normal lives”.
A Nigerian study of 74 patients starting ARVs found that they gained an
average of 12kgs in 24 weeks.
In May and June, I spent six weeks with a group of women preparing to go on
ARVs at iThemba Clinic in Mariannhill outside Durban. At the beginning of
the six-week treatment training course, most were thin and constantly
shivering. Every week, at least one of the 10 women had been hospitalised.
The transformation in the women after a few weeks on treatment has been
remarkable, both in terms of weight gain and improved health as well as a
sense of psychological well-being as they have been freed from the burden of
staring death in the face.
As ARVs boost people’s immunity, making them less prone to infections,
health workers will have to treat less AIDS patients. This will make more
room for non-AIDS patients, particularly the elderly and children who have
been “crowded out” by AIDS patients, according to a recent study by the
Human Sciences Research Council (HSRC).
But at the same time, there are immense dangers. If the programme is not
properly implemented, it could result in multi-drug resistant HIV that will
not respond to any known ARV drugs.
The success of the programme relies on enrolled patients taking their drugs
properly and at the same time every day 95% of the time. Proper patient
adherence relies on a number of things, including adequate support from
their families.
The country’s longest running ARV programme, the Medicins sans Frontieres’
Khayelitsha programme, will not give drugs to people who have not disclosed
their HIV status to at least one member of their household.
“Disclosure lightens the psychic burden. Often people don’t have the mental
energy to tackle adherence if they are trying to deal with the knowledge of
their HIV status on their own,” says Wilson.
However, government will not be able to impose such a condition. According
to former director general of health, Dr Ayanda Ntsaluba, lawyers have told
the department that people will only be allowed to be excluded for “factors
within their control, such as drug and alcohol abuse”.
Drug resistance is already a problem in countries that have had ARV
treatment for some time. In July this year, researchers at the Paris HIV
Pathogenesis Conference reported on a study of 1 600 people from 17 European
countries. All were newly diagnosed with HIV and had never taken ARVs, yet
10% had strains of HIV that were already resistant to ARVs. This suggests
that they were infected with drug-resistant HIV from people who had not been
taking their ARVs properly, thus causing their virus to become resistant.
This chilling report underscores the importance of treatment needing to go
hand-in-hand with prevention efforts. South Africa cannot afford to divert
resources from prevention to pay for treatment. One effort cannot succeed
without the other.
Successful ARV programmes also rely on a contract between health providers
and patients, says Wilson. “Patients have to be empowered to take their
medication. They have to understand what they are doing as they have to do
it for the rest of their lives,” he says.
At iThemba clinic, trainer Zinhle Thabete tells potential patients: “I never
want to hear you talking about ‘those little yellow pillies’. You need to
know the names of your drugs and what their side effects can be. You also
need to have a treatment plan and know exactly when you are going to take
the drugs.”
Wilson smiles when I ask about the challenges that lie ahead: “A Chinese
saying keeps going through my head,” he says. “The gods grant the wishes of
those it wants to punish!”
E-mail Kerry Cullinan
Author

Kerry Cullinan is the Managing Editor at Health-e News Service. Follow her on Twitter @kerrycullinan11
Republish this article
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Unless otherwise noted, you can republish our articles for free under a Creative Commons license. Here’s what you need to know:
You have to credit Health-e News. In the byline, we prefer “Author Name, Publication.” At the top of the text of your story, include a line that reads: “This story was originally published by Health-e News.” You must link the word “Health-e News” to the original URL of the story.
You must include all of the links from our story, including our newsletter sign up link.
If you use canonical metadata, please use the Health-e News URL. For more information about canonical metadata, click here.
You can’t edit our material, except to reflect relative changes in time, location and editorial style. (For example, “yesterday” can be changed to “last week”)
You have no rights to sell, license, syndicate, or otherwise represent yourself as the authorized owner of our material to any third parties. This means that you cannot actively publish or submit our work for syndication to third party platforms or apps like Apple News or Google News. Health-e News understands that publishers cannot fully control when certain third parties automatically summarise or crawl content from publishers’ own sites.
You can’t republish our material wholesale, or automatically; you need to select stories to be republished individually.
If you share republished stories on social media, we’d appreciate being tagged in your posts. You can find us on Twitter @HealthENews, Instagram @healthenews, and Facebook Health-e News Service.
You can grab HTML code for our stories easily. Click on the Creative Commons logo on our stories. You’ll find it with the other share buttons.
If you have any other questions, contact info@health-e.org.za.
No turning back
by Kerry Cullinan, Health-e News
September 25, 2003