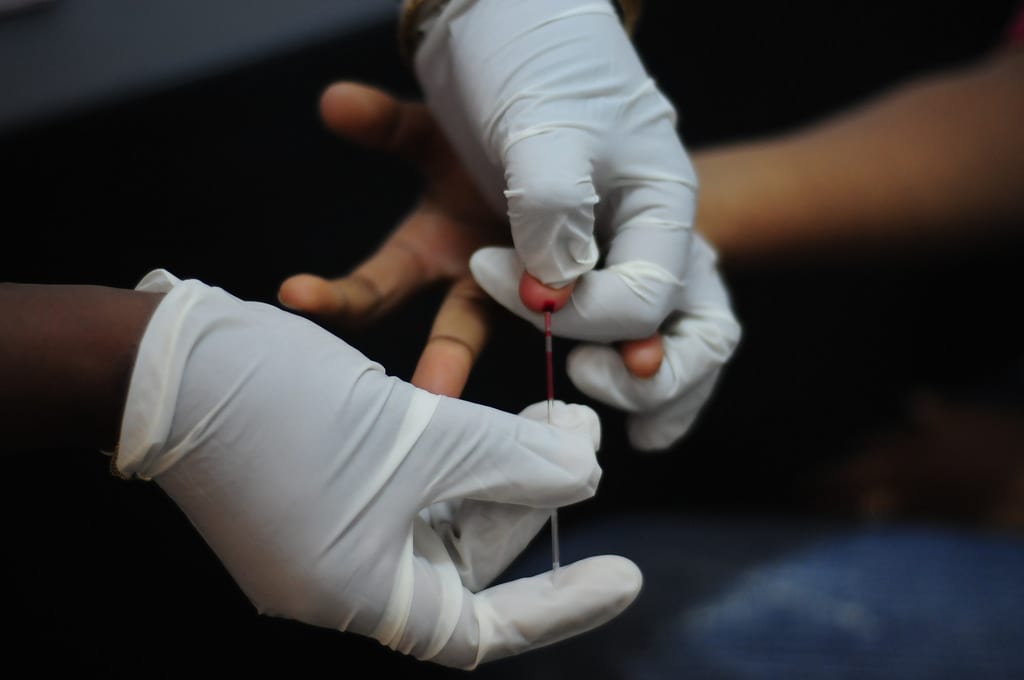
Half of the almost 1 600 children who died in 15 hospitals in 2005 were clinically eligible for antiretroviral medication yet only 3 percent ‘ a total of 48 children ‘ were on ARVs.
Almost half had never been tested for HIV, and only seven percent of the dead children’s mothers were known to have been given the antiretroviral drug nevirapine to prevent HIV positive mothers from infecting their babies.
These are some of the findings of the report, ‘Saving Children 2005’ compiled by the Child Problem Identification Programme and the Medical Research Council, based on information supplied by 15 hospitals in six provinces over a period of five months.
The low rate of HIV testing, and the poor reach of the prevention of mother-to-child HIV transmission (PMTCT) and antiretroviral programmes represent ‘missed opportunities for improving the care of children in South Africa’, writes Dr Neil McKerrow, a specialist paediatrician with the KwaZulu-Natal health department.
‘An awareness of HIV infection in children is obviously present but needs to be converted into positive action,’ he added.
Coronation Hospital in Newclare, Johannesburg, was an exception to the rule, as only 12.5% of its child patients died without having been tested.
Despite over 70% of its child patients being both HIV positive and underweight or malnourished, Coronation managed to keep its child mortality down to 4.2%.
It attributes its success to an extremely well-motivated paediatric team.
KwaZulu-Natal paediatrician Dr Kimesh Naidoo writes that the establishment of the PMTCT programmes ‘have not decreased the number of infected newborn infants’ in his province.
The report recommends that all babies are given an HIV test when they come for their first vaccination visit at six weeks old, while all children who are hospitalised should routinely be tested for HIV.
Malnutrition also had a severe effect on children’s health. Six out of every to children who died were underweight and over half of these had severe malnutrition.
Only 12% of underweight children who were tested for HIV were negative and only 4% of children with marasmus who were tested were negative.
‘This demonstrates the tremendous overlap of HIV infection and severe malnutrition in South African children,’ notes the report.
It recommends that improved feeding and poverty alleviation ‘must go hand in hand with ARV access’ for children. It also calls for an audit of clinic-based nutrition services to find out what the barriers are to children getting nutrition.
Almost seven percent of all children who were hospitalised died, with the most deaths in children aged between one month and a year old.
The main causes of death were respiratory infections (eg pneumonia), septicaemia (generalised infection circulating in the blood stream), diarrhoea, an HIV-related pneumonia called pneumoncystis pneumonia (PCP) and tuberculosis. The TB rate has almost doubled in a single year.
KwaZulu-Natal hospitals had the highest death rate, with almost 10 percent of children at Grey’s Hospital dying. However, Kalafong Hospital also had a high death rate of 9.,8 percent.
One in three babies died within 24 hours of admission. This meant that children were often brought to the hospital too late to be treated successfully. Bt it also meant that they were admitted
However, there were also a number of problems in the way they were treated.
At clinic level, the vast majority of problems lay with the failure of healthworkers to assess, treat and refer children appropriately.
At hospitals, barriers to children’s care on admission rested with the lack of beds, senior doctors and paediatric intensive care units.
In the wards themselves, the top three factors contributing to the deaths of the children were inadequate monitoring of blood glucose, inappropriate antibiotics or TB treatment and incorrect intravenous fluid.
Three quarters of the problem areas in wards related to clinical staff, with insufficient monitoring and assessment the biggest problem.
When assessing 322 deaths in their own hospitals, healthworkers reported that 146 (45%) were ‘avoidable’.
Poor record-keeping was noted
Reported staff shortages increased ‘enormously’ from 41 reports to 233 reports in the space of a year.
Reports on a lack of bed and overcrowding more than doubled in a year.
‘Child health will not significantly improve until the HIV epidemic is controlled and reversed. This must be the absolute priority,’ notes the report. ‘ Health-e News Service.