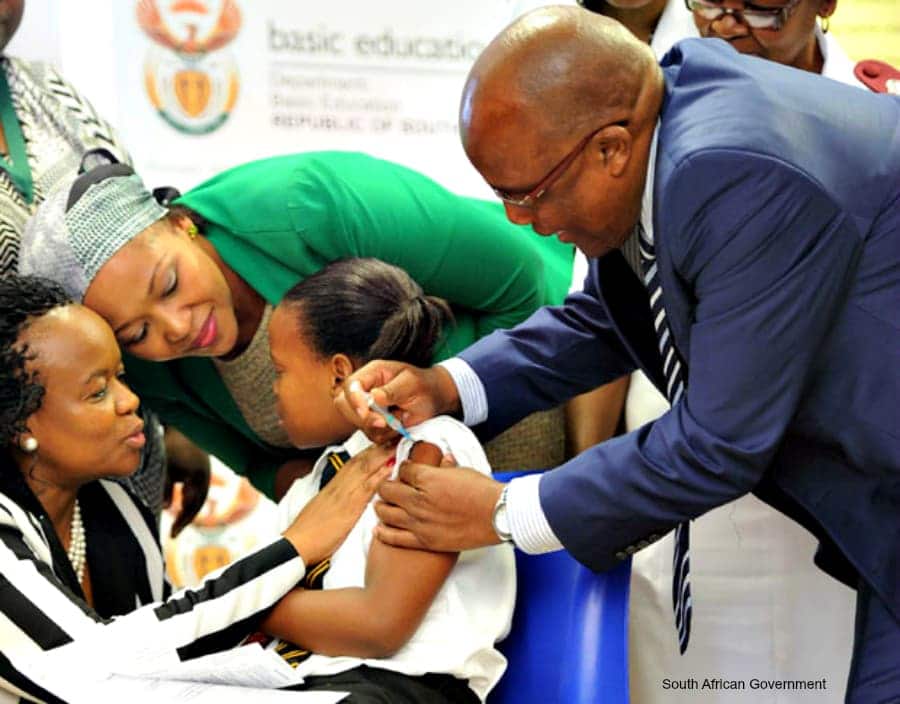
Male circumcision and reducing multiple partners the way to go
Policy analysis led by researchers at the Harvard School of Public Health (HSPH) and the University of California, Berkeley, found that the most common HIV prevention strategies – condom promotion, HIV testing, treatment of other sexually transmitted infections (STIs), vaccine and microbicide research, and abstinence are having a limited impact on the predominantly heterosexual epidemics found in Africa.
The researchers also said some of the assumptions underlying such strategies such as poverty or war being major causes of AIDS in Africa are unsupported by rigorous scientific evidence.
‘Two interventions currently getting less attention and resources- male circumcision and reducing multiple sexual partnerships – would have a greater impact on the AIDS pandemic and should become the cornerstone of HIV prevention efforts in the high-HIV-prevalence parts of Africa,’ the researchers argued.
The research paper appears in the journal Science this week.
‘Despite relatively large investments in AIDS prevention efforts for some years now, including sizeable spending in some of the most heavily affected countries (such as South Africa and Botswana), its clear that we need to do a better job of reducing the rate of new HIV infections. We need a fairly dramatic shift in priorities, not just a minor tweaking,’ said Daniel Halperin, lecturer on international health in the HSPH Department of Population and International Health and one of the paper’s lead authors.
The AIDS pandemic continues to devastate some populations worldwide.
In most countries, HIV transmission remains concentrated among sex workers, men who have sex with men and/or injecting drug users and their sexual partners.
In many parts of Africa, especially sub-Saharan Africa, HIV has jumped outside these high-risk groups, creating generalised epidemics spread mainly among people who are having multiple and typically concurrent (overlapping, longer-term) sexual relationships.
In nine countries in southern Africa, more than 12% of adults are infected with HIV.
The authors said that the current widely used prevention strategies, while having value in some instances, are not as effective at preventing HIV transmission as male circumcision and reducing multiple sexual partners and thus should not continue to receive the bulk of donor investments for prevention, especially in Africa.
They cited the example of Thailand where condom use is widely promoted as an HIV prevention measure and is effective as the epidemic is spread primarily through sex work.
‘However, studies have found no evidence that condom use has played a primary role in HIV decline in generalized, primarily heterosexual epidemics, such as those in southern Africa,’ the authors said.
They said this was mainly because most HIV transmission there occurs in more regular sexual relationships, in which achieving consistent condom use has proved extremely difficult.
‘The evidence is similarly lacking for other popular prevention approaches as well,’ Halperin and his nine co-authors said.
Studies have shown no consistent reduction in risk for those testing HIV-negative and testing programs have produced no evidence of HIV reduction in populations, they said.
‘The treatment of other STIs has had discouraging results; vaccine development trials and microbicide testing have been disappointing; and abstinence is not likely to have a major impact since most HIV infections occur among people in their 20s or older, when most are already sexually active,’ they said.
The authors pointed out that in contrast, many studies in the last two decades have shown that male circumcision significantly reduced the risk of heterosexual HIV infection.
In west Africa, where male circumcision is widespread, the prevalence of HIV remains relatively low.
When initial findings from three recent randomized controlled trials of male circumcision in Africa showed at least a 60% reduction in HIV risk, the trials were stopped early because it was not ethical to withhold the clearly proven benefits of this simple surgical procedure.
‘It is tragic that we did not act on male circumcision in 2000, when the evidence was already very compelling. Large numbers of people will die as a result of this error,’ said Malcolm Potts, co-lead author and Bixby Professor of Population and Family Planning at UC Berkeley School of Public Health.
Similarly, partner reduction appears to have played a primary role in reducing HIV rates in Uganda, Kenya, Zimbabwe, Cote dIvoire, and in urban Malawi and Ethiopia.
Ugandas Zero Grazing campaign, initiated in 1987, indicated that reducing partners can be achieved on a large scale as later surveys revealed that the number of people reporting multiple and casual partners declined by over half.
‘The political fight in the United States between supporters of condoms and supporters of abstinence has obscured the importance of what is arguably the most powerful of what are known as the three ABC strategies (Abstinence, Be Faithful, Condoms), which is the B, or partner reduction and fidelity aspect,’ according to the papers authors.
The authors also argued that HIV prevention priorities needed to shift significantly to reflect the best available scientific evidence. They noted that only 1% of total prevention funding requested by the United Nations AIDS Program is earmarked for male circumcision, and that reducing multiple sexual partnerships would probably garner only a small fraction of community mobilization and mass media, workplace or other HIV prevention investments.
The vast majority of donor investments in HIV prevention in the generalized epidemics of Africa continue to go to approaches for which the evidence of actual impact is increasingly unclear, said Halperin.
‘Many of these approaches, such as HIV testing and treating other STIs, do have important public health benefits, and should be continued, but not because we believe they will definitely have a major impact on reducing HIV infections,’ he said.
Author

Kerry Cullinan is the Managing Editor at Health-e News Service. Follow her on Twitter @kerrycullinan11
Republish this article
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Unless otherwise noted, you can republish our articles for free under a Creative Commons license. Here’s what you need to know:
You have to credit Health-e News. In the byline, we prefer “Author Name, Publication.” At the top of the text of your story, include a line that reads: “This story was originally published by Health-e News.” You must link the word “Health-e News” to the original URL of the story.
You must include all of the links from our story, including our newsletter sign up link.
If you use canonical metadata, please use the Health-e News URL. For more information about canonical metadata, click here.
You can’t edit our material, except to reflect relative changes in time, location and editorial style. (For example, “yesterday” can be changed to “last week”)
You have no rights to sell, license, syndicate, or otherwise represent yourself as the authorized owner of our material to any third parties. This means that you cannot actively publish or submit our work for syndication to third party platforms or apps like Apple News or Google News. Health-e News understands that publishers cannot fully control when certain third parties automatically summarise or crawl content from publishers’ own sites.
You can’t republish our material wholesale, or automatically; you need to select stories to be republished individually.
If you share republished stories on social media, we’d appreciate being tagged in your posts. You can find us on Twitter @HealthENews, Instagram @healthenews, and Facebook Health-e News Service.
You can grab HTML code for our stories easily. Click on the Creative Commons logo on our stories. You’ll find it with the other share buttons.
If you have any other questions, contact info@health-e.org.za.
Male circumcision and reducing multiple partners the way to go
by Kerry Cullinan, Health-e News
May 9, 2008