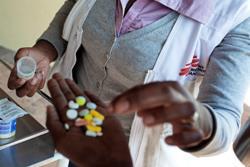
Stock-outs, low awareness stymie immunisations


“Growing up, we were not allow to say “measles,” or incubulujwane, around young children because it was believed that they would get sick or even die immediately from it,” said Sarah Maluleka from Ermelo, about 210 kilometres southwest of Nelspruit. “Our parents believed that measles was a traditional illness and we were made to believe the same thing.”
“Knowing that a child needs to be immunised is new,” Maluleka told OurHealth.
Gert Sibande district, under which Ermelo falls, has the country’s 11th worst vaccination rate. In 2012, only about half of children there had been fully vaccinated by the age of one year, according to the District Health Barometer.
A recent Health-e investigation in Gauteng, the Eastern Cape and Limpopo found that vaccine stock outs and storage problems are helping fuel poor vaccination rates.
When a clinic runs out of vaccines, mothers like Gloria Ndlovu who are keen to have their children vaccinated on time have no choice but to spend more money to return to the clinic another day or travel to a neighbouring clinic.
“Being ask to come the following day is not possible for me because I live far from the facility and I have to pay for transport,” said Ndlovu, who is unemployed and has a 13-month-old baby. “The lucky mothers are those living in the township – at least they have two health facilities to choose from.”
Turned away
Ermelo Town Clinic vaccinates an average of 25 children a month and six of its nurses have been trained to immunise children. In the case of a stock-out, nurses can place emergency orders but they admit that it still means some mothers will have to make an extra trip back to the clinic.
“If it happens that we run out of vaccines, we have the option to use the emergency order system and order through the district pharmacist,” said one health worker who spoke on condition of anonymity. “Then we have to apologise to the mothers and ask them to come the following day.”
[quote float=”left”]”The lucky mothers are those living in the township – at least they have two health facilities to choose from”
At Eziweni Clinic in Daantjie, about 30 kilometres outside Nelspruit, only one nurse has been trained to immunise children. In late February, the clinic was forced to turn mothers away while this nurse attended an offsite meeting.
Nurses at the clinic also reported that they had been experiencing stock-outs of vaccines and other medicines for three weeks.
“We placed an order with the provincial depot in Middleburg and made follow-ups but still no medication has been delivered,” said one health worker. “Unfortunately most of the parents who are turned away don’t even know the implication of not giving a child the necessary vaccines.”
One of those mothers is Nombusa Masinga, who is living with HIV and had brought her 18-month-old baby girl for her measles booster and final HIV test as part of prevention of mother-to-child HIV transmission (PMTCT) services.
“I don’t know what this means or what kind of illness she will have if she doesn’t receive her vaccination,” she told OurHealth. “Some were told to come back tomorrow.”
Babies can contract HIV from their mothers before or during birth or through breastfeeding if the mother is not on antiretrovirals (ARVs) for their own health or as part of prevention of mother-to-child transmission services. Babies born to women living with HIV should be tested for HIV six weeks after birth, six weeks after weaning and at 18 months of age, according to the country’s 2013 PMTCT guidelines.
Missing booster shots
Many vaccinations are given in two doses, several months apart. Children should be vaccinated for measles at nine and then 18 months, but about 15 percent of babies in Gert Sibande never make it back for their second measles shot, according to the District Health Barometer.
[quote float=”right”]“Nurses must tell us what kind of a vaccine they are giving our children. I have the right to know what is being given to my baby”
According to Ermelo nurses, children may miss their second measles dose because mothers are working and there is no one else to take the child to the clinic — or because the “Road to Health” cards that track the child’s immunisations is lost.
Many mothers may also not understand how important immunisations and may not even know which vaccines nurses are administering to babies, says Lindiwe Ngomane, who has a seven-month-old baby.
“Mothers and care givers needs to be educated about the importance of immunisation for children…because some of us don’t know how to read,” Ngomane tells OurHealth. “I honestly believe that when we take our children to the facility to be immunised that the nurses must tell us what kind of vaccine they are giving our children.”
“I have the right to know what is being given to my baby,” she adds.
Read more from Health-e’s investigation into vaccination in South Africa “Shots in the dark?” as part of the African Story Challenge:
- Shots in the dark? Vaccines in South Africa
- Shots in the dark? Snapshots of Health-e investigation
- Film: Shots in the Dark? A look at vaccines in the Eastern Cape
- Missing babies, missing booster shots in the Eastern Cape
- Stock-outs, low awareness stymie immunisations
- Vaccinations are everyone’s business in Shoshanguve
- What is measles?
Author
Republish this article
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Unless otherwise noted, you can republish our articles for free under a Creative Commons license. Here’s what you need to know:
You have to credit Health-e News. In the byline, we prefer “Author Name, Publication.” At the top of the text of your story, include a line that reads: “This story was originally published by Health-e News.” You must link the word “Health-e News” to the original URL of the story.
You must include all of the links from our story, including our newsletter sign up link.
If you use canonical metadata, please use the Health-e News URL. For more information about canonical metadata, click here.
You can’t edit our material, except to reflect relative changes in time, location and editorial style. (For example, “yesterday” can be changed to “last week”)
You have no rights to sell, license, syndicate, or otherwise represent yourself as the authorized owner of our material to any third parties. This means that you cannot actively publish or submit our work for syndication to third party platforms or apps like Apple News or Google News. Health-e News understands that publishers cannot fully control when certain third parties automatically summarise or crawl content from publishers’ own sites.
You can’t republish our material wholesale, or automatically; you need to select stories to be republished individually.
If you share republished stories on social media, we’d appreciate being tagged in your posts. You can find us on Twitter @HealthENews, Instagram @healthenews, and Facebook Health-e News Service.
You can grab HTML code for our stories easily. Click on the Creative Commons logo on our stories. You’ll find it with the other share buttons.
If you have any other questions, contact info@health-e.org.za.
Stock-outs, low awareness stymie immunisations
by cynthiamaseko, Health-e News
March 11, 2014