Study links birth control to increased risk of HIV infection

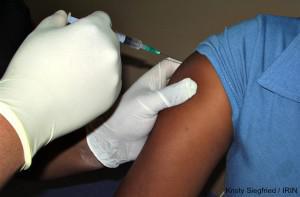
Researchers have questioned a possible link between hormonal contraception use and HIV risk since 1991. Only 20 years later did a 2011 study published in the international medical journal The Lancet showing that “the shot” doubled women’s risk of both contracting and transmitting the virus prompt a World Health Organisation (WHO) review of the evidence.
The WHO affirmed the birth control method’s safety, but strongly recommended women on progesterone-only injections, like Depo-Provera, also use condoms to prevent HIV infection.
The study also refuelled a divisive and sometimes ugly debate within the scientific community, which remains divided on the issue and evidence.
To wade through the evidence, US University of California Berkley researchers looked at 12 published studies examining possible HIV risk associated with hormonal contraception. The bulk of these studies were conducted at least partially in South Africa.
According to the research published in The Lancet, the pooled results of these studies showed that women had about a 30 percent increased risk of contracting HIV when using the injectable hormonal contraception depot medroxprogeterone acetate.
More commonly known by the brand name Depo-Provera, this birth control shot increased likelihood of at-risk women such as sex workers and those in HIV-positive men by 40 percent, according to lead author Lauren Ralph.
Women cautioned not to ditch the shot just yet
Ralph stresses that her findings should not prompt women to ditch the popular contraception method just yet.
[quote float = right] “Although we do observe a moderately increased risk of HIV among Depro users, we don’t feel our findings justify the withdrawal of Depro in most settings”
“Although we do observe a moderately increased risk of HIV among Depro users, we don’t feel our findings justify the withdrawal of Depro in most settings worldwide” Ralph told Health-e News. “Banning Depro would leave many women without access to contraception and, because child birth remains life threatening in many places, this could increase the overall number of deaths among women.”
She added that no studies suggested any increased HIV risk associated with using the injectable contraceptive Norethisterone enanthate, commonly known as NET-EN.
Instead, Ralph said her results may help mathematical modellers determine what adding or removing the birth control shot from national programmes might mean both for new HIV infections and maternal deaths.
Completed as part of her dissertation in epidemiology, Ralph’s research also highlights the dearth of research examining the relationship between hormonal contraception and HIV in high-risk women. Only two out of the 12 studies ultimately included in the analysis were conducted among these groups
In South Africa, about one in every 1000 live births result in a mother dying. While some countries in east and southern Africa have contemplated removing Depo-Provera from national programmes, South Africa’s latest contraception guidelines continue to include the birth control method but caution women on Depo-Provera to also use condoms as per WHO advice.
Study is the latest evidence in a heated – and sometimes dirty – debate
According to University of Cape Town professor Dr Christopher Colvin, Ralph’s meta-analysis adds important data to what has been what he calls an increasing narrow and fierce debate about hormonal contraception’s possible HIV links.[quote float= left]“The stakes are high, the evidence is murky… policies, budgets, careers and reputations are at stake”
“Like many scientific controversies, views have become hardened, personal, financial, or political agendas have been suggested, and there has even been intrigue in the form of leaked copies of articles under peer review,” wrote Colvin in a related commentary piece.
Fiery debate is fuelled by the multiple threats that the debate poses to women’s health and the siloed nature of the health community.
“The stakes are high, the evidence is murky…and many people/organisations work in disease-specific ‘silos’… a fact that makes them less likely to engage with each other consistently and productively,” he added. “Policies, budgets, careers and reputations are at stake.”
The debate has also turned dirty with peer reviewers leaking unpublished studies to advocacy groups “with axes to grind,” he told Health-e News.
The scientific community is also at odds about whether the scientific “gold standard,” a randomised controlled clinical trial, could ever take place practically and ethically. Colvin argues that whether or not to hold a clinical trial and what to do with what we know now are two separate conversations.
“Ultimately, it may be that a trial adds an important layer to our evidence that points us in a clearer direction but it isn’t likely to suddenly answer all of our questions,” said Colvin, adding that a trial would take at least four years to produce results. “We need to be thinking about all of the evidence at the same time, and all of the different decisions we need to make now and in the future.” – Health-e News
Author
Republish this article
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Unless otherwise noted, you can republish our articles for free under a Creative Commons license. Here’s what you need to know:
You have to credit Health-e News. In the byline, we prefer “Author Name, Publication.” At the top of the text of your story, include a line that reads: “This story was originally published by Health-e News.” You must link the word “Health-e News” to the original URL of the story.
You must include all of the links from our story, including our newsletter sign up link.
If you use canonical metadata, please use the Health-e News URL. For more information about canonical metadata, click here.
You can’t edit our material, except to reflect relative changes in time, location and editorial style. (For example, “yesterday” can be changed to “last week”)
You have no rights to sell, license, syndicate, or otherwise represent yourself as the authorized owner of our material to any third parties. This means that you cannot actively publish or submit our work for syndication to third party platforms or apps like Apple News or Google News. Health-e News understands that publishers cannot fully control when certain third parties automatically summarise or crawl content from publishers’ own sites.
You can’t republish our material wholesale, or automatically; you need to select stories to be republished individually.
If you share republished stories on social media, we’d appreciate being tagged in your posts. You can find us on Twitter @HealthENews, Instagram @healthenews, and Facebook Health-e News Service.
You can grab HTML code for our stories easily. Click on the Creative Commons logo on our stories. You’ll find it with the other share buttons.
If you have any other questions, contact info@health-e.org.za.
Study links birth control to increased risk of HIV infection
by lauralopez, Health-e News
January 12, 2015



