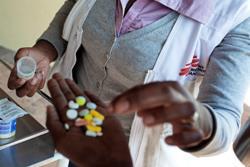
A family’s cycle of sex work


To her, her mother was a strong woman and a best friend who kept a roof over their heads during tough times – but from an early age, she knew their family was a bit different.
“After we lost our house when I was young, we started moving from house to house,” says Ndlovu who grew up in KaMsogwaba in Nelspruit and now lives in Witbank. “While my friends’ parents went to work every morning, my mother worked at night.”
By 11 years of age, Ndlovu had started drinking and smoking – exploiting the fact that her mother worked nights and often slept during the day to get into her alcohol.
“Every time she sent me to buy her alcohol and cigarettes, she would pay me first,” she tells OurHealth. “Smoking was easy because I was buying my own cigarettes with the little money I had.”
Even she was surprised at her mother’s reaction when she caught her smoking in the toilet two years later. She thought she would be beaten. Instead, Ndlovu began drinking and smoking with her mother and her friends.
[quote float=”right”]“My biggest inspiration is my daughter – I don’t want her to grow up in the same situation I was in”
“Every time my mother and her friends were drinking, I would join them,” she remembers. “My mother said it was better for me to drink with them than to drink with people she didn’t know.”
“My mother and I became best friends,” she adds. “Everywhere she went, I would follow.”
But the “friendship” soon soured as the mother and her teenage daughter began having sharing sexual partners while drunk. By 17 years old, Ndlovu says she was done with a life that was going nowhere – and that was putting the baby growing in her belly at risk.
“I was so tired of living like there was no tomorrow,” she says. “I found out I was pregnant and HIV-positive.”
“I tried to change for my unborn baby but couldn’t because I was still living with mother,” she adds. At 19 years old, Ndlovu was a runaway living with a boyfriend 20 years her senior who was working on the mines. The relationship was short-lived, and soon young mother and child were out on the streets.
“I had no job and I started selling my body just to have a place to sleep and food,” Ndlovu says.
Sex work provides but no path for daughter
[quote float=”left”]”In four years in this business, I have managed to buy my own house, and put my daughter and myself in school”
Ndlovu continues to work as a sex worker and says most of her clients are miners or truckers. While she has been able to make a better life for herself and her child, she says she still keeps her work a secret from friends and her daughter.
“In four years in this business, I have managed to buy my own house and put my daughter and myself in school,” she says. “My biggest inspiration is my daughter – I don’t want her to grow up in the same situation I was in.”
She asked to remain anonymous for this story. Even so, Ndlovu says her job as a sex worker does not define her.
“My work doesn’t reflect me,” Ndlovu adds. “I am like any woman you know.”
Ndlovu, who has not yet started antiretrovirals (ARV), says she uses condoms to protect her clients from contracting HIV as well as herself from re-infection in which people living with HIV can contract additional strains of the virus that may complicate treatment and lead to drug resistance.
Taking ARVs can reduce the risk that people living with HIV will transmit the virus to their sexual partners.
In 2011, results from the HPTN-052 study found that people who initiated ARVs early and had an undetectable viral load, or small amount of virus in their blood, were about 96 percent less likely to transmit HIV to their partner. Based on that research, some countries in southern Africa have moved to provide groups at high risk of HIV like sex workers and men who have sex with men earlier access to HIV treatment in hopes of preventing new infections.
While recent estimates are not available for the HIV prevalence among South African sex workers, previous research has found an HIV prevalence of as much as 69 percent among the group.
Thanks to prevention of mother-to-child HIV transmission services, Ndlovu’s daughter was born HIV negative.
Still close with her own mother, Ndlovu says she hopes her daughter will never know what she does to provide for the two – and that she will be the first in two generations to make her money a different way. – Health-e News Service.
*Name changed to protect the woman’s identity
Author
Republish this article
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Unless otherwise noted, you can republish our articles for free under a Creative Commons license. Here’s what you need to know:
You have to credit Health-e News. In the byline, we prefer “Author Name, Publication.” At the top of the text of your story, include a line that reads: “This story was originally published by Health-e News.” You must link the word “Health-e News” to the original URL of the story.
You must include all of the links from our story, including our newsletter sign up link.
If you use canonical metadata, please use the Health-e News URL. For more information about canonical metadata, click here.
You can’t edit our material, except to reflect relative changes in time, location and editorial style. (For example, “yesterday” can be changed to “last week”)
You have no rights to sell, license, syndicate, or otherwise represent yourself as the authorized owner of our material to any third parties. This means that you cannot actively publish or submit our work for syndication to third party platforms or apps like Apple News or Google News. Health-e News understands that publishers cannot fully control when certain third parties automatically summarise or crawl content from publishers’ own sites.
You can’t republish our material wholesale, or automatically; you need to select stories to be republished individually.
If you share republished stories on social media, we’d appreciate being tagged in your posts. You can find us on Twitter @HealthENews, Instagram @healthenews, and Facebook Health-e News Service.
You can grab HTML code for our stories easily. Click on the Creative Commons logo on our stories. You’ll find it with the other share buttons.
If you have any other questions, contact info@health-e.org.za.
A family’s cycle of sex work
by cynthiamaseko, Health-e News
July 24, 2014